Types of Gastric Cancer :
- Adenocarcinoma - most common type, accounts for 90-95% and develops in gastric glands.
- Gastric lymphoma – which arise from lymphoid area of stomach.
- Gastric Leiomyosarcoma - very rare presentation, arises from connective tissues of gastric wall.
- Gastrointestinal Tumors ( GIST )
- Neuroendocrine Tumors
If stomach cancer is diagnosed at an early stage, there is a good chance of a cure. In general, the more advanced the cancer (the more it has grown and spread), the less chance that treatment will be curative.
Risk factors of Gastric Malignancy
- Age - common in older people of age group >55 years
- Sex – male and female ratio is 2:1
- Pernicious Anemia - an autoimmune disease where the stomach does not produce intrinsic factor for absorption of Vitamin B12 which also causes anaemia.
- Dietary factors ( GIST ) diet containing lot of salt, pickled and smoked foods. Diet lack of lots of fruit and green vegetables.
- Blood group A - slightly higher incidence in people with blood group A.
- Smoking – higher incidence of gastric cancer in smokers.
- Helicobacter pylori infection - long standing H. pylori infection to gastric mucosal layer is associated with gastric ulcers and chronic atrophic gastritis which is associated with the high incidence of gastric cancer.
- Family history – some genetic diseases run in family like hereditary nonpolyposis colorectal cancer, familial adenomatous polyposis, and PeutzJeghers syndrome which all predispose to gastric cancer.
Symptoms of Gastric cancer
Majority of the patients with early stage of gastric cancer present nonspecific symptoms resembling that of peptic ulcer disease, however some do not cause any symptoms until they are quite advanced.
Symptoms include -
- Pain or discomfort in the upper abdomen after meal.
- Dyspepsia – a sense of fullness after eating, belching, indigestion.
- Weight loss.
- Loss of appetite & weakness.
- Malena - black stool.
- Anemia – become evident if tumor bleeds.
- Recurrent vomiting after meal - if the tumor is situated in the distal part of stomach and obstructing the lumen.
- Dysphagia– difficulty in swallowing in cases of the tumor arising from proximal part of stomach obstructing the meeting point of stomach and esophagus (food pipe).
- Hematemesis - vomiting blood is less common symptom.
Diagnosis of Gastric cancer
The patient is evaluated on the basis of history, symptoms and clinical signs. Along with routine blood test and X-ray some endoscopic and radiological investigations are done which include:
- Upper gastrointestinal endoscopy - the endoscope is a small diameter flexible tube which is passed through the mouth, into the esophagus and down towards the stomach to examine the inner lining of stomach and any growth arising from gastric mucosa.
- Endoscopic Biopsy - if anything abnormal is seen during endoscopy over mucosal lining, a small piece of tissue is taken to confirm the diagnosis. The sample is then examined under the microscope to look for cancer cells. IHC for HER2 is important here for prognostication and selecting anti-cancer agent.
- Endoscopic ultrasound (EUS): An endoscope with a small ultrasonic probe at its tip is used for the assessment for early gastric cancer. As very early Gastric cancers can be treated endoscopically, this investigation has paramount importance.
- Barium meal x- ray thin barium is used to swallow which outline the tumor inside the stomach, though is a seldom done these days.
- CT scans of the abdomen and chest - are done for the local assessment of gastric tumor as well as to rule out spread to distant organs, like the liver and lungs and spread to lymph nodes close to the stomach.
- PET scan – is done to rule out distant spread (metastasis) if there is a suspicion.
- Staging Laparoscopy - used for the staging gastric cancer. A telescope is introduced inside the abdomen which directly visualize entire abdominal cavity and organs adjacent to stomach. This is an important test done before stating any therapy because sometimes it can alter the plan.
- Serum CEA (carcinoembryonic antigen) estimation – This substance is released into the bloodstream from both cancer cells and normal cells. A higher level than normal amounts suggest a sign of gastric cancer.
Treatment options for Gastric cancer:
Treatment options include surgery, chemotherapy and sometimes radiotherapy. The treatment is advised for each case depends upon the stage of the disease and the general condition of the patient.
Endoscopic Management:
Endoscopic mucosal resection (EMR) and Endoscopic submucosal dissection (ESD) are the treatment for early gastric cancer (tumor involves the mucosal layer). If the histopathological examination of the resected specimen shows incomplete resection or deep invasion by tumor then the patient would need a formal resection (removal by surgery).
Surgery:
 Surgery is the most definitive treatment. Surgery is always required for curative treatment. Part or all of the stomach, as well as the surrounding lymph nodes are removed, with the basic goal of removing all cancer and a margin of normal tissue. Depending on the extent of invasion and the location of the tumor, surgery may also include removal of part of the intestine or pancreas.
Surgery is the most definitive treatment. Surgery is always required for curative treatment. Part or all of the stomach, as well as the surrounding lymph nodes are removed, with the basic goal of removing all cancer and a margin of normal tissue. Depending on the extent of invasion and the location of the tumor, surgery may also include removal of part of the intestine or pancreas.
This can be done by either open or minimal invasive methods. Minimal invasive method of gastric cancer resection is getting more popular now a day because of its low operative morbidity, shorter hospital stay and similar oncological outcomes.
Management (Options of surgery, Chemotherapy and radiotherapy) depends on clinical staging of gastric tumors.
Stage 0 (Carcinoma in Situ):
- Endoscopic surgery - Endoscopic mucosal resection(EMR) or Endoscopic submucosal dissection (ESD).
- Minimal access or open surgery - total or subtotal gastrectomy depending on the location of tumor in stomach.
Stage I & II Gastric Cancer:
Minimal access or open surgery - total or subtotal gastrectomy depending on the location of tumor in stomach.
Stage III Gastric Cancer:
- Minimal access or open surgery - total or subtotal gastrectomy depending on the location of tumor in stomach.
- Chemotherapy & radio therapy given before and after surgery.
Stage IV and Recurrent Gastric Cancer:
- Palliative Surgery on stomach is to stop bleeding from stomach or to bypass the distal blockade of stomach.
- Chemotherapy and radiotherapy (rarely) are used as palliative therapy to relieve symptoms and improve the general condition of the patients.
- Endoscopic laser and end luminal stenting to relieve gastric outlet obstruction.
Chemotherapy
Chemotherapy may be given before surgery (neoadjuvant) to down stage the disease or after the surgery (adjuvant) to reduce risk of recurrence. In chemotherapy, anticancer medicines are used to kill cancer cells. The standard chemotherapy is the combination of 5-FU and leucovorin. Second line chemotherapy drugs are cisplatin, oxaloplatin and epirubicin are also used in advanced gastric cancer. Newer regimens are FLOT or FOLFOX are used more often now.
Biological Therapy
Patients with metastatic gastric or gastroesophageal (GE) junction adenocarcinoma with HER2 overexpressing, trastuzumab (Herceptin) in combination with cisplatin and a fluoropyrimidine (capecitabine or 5-fluorouracil) is used.
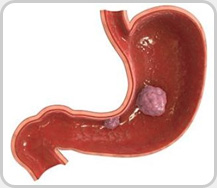
 The stomach is a hollow muscular organ, part of proximal digestive system and located on the left side of the upper abdomen below rib cage. The stomach receives food from the esophagus. It secretes acid and digestive enzymes. Gastric cancer also known as stomach cancer arises from the inner lining (mucosa) of stomach. Early gastric cancer involve only inner layer (mocosa) while in advance stage it involves more deeply into the stomach wall and spread to surrounding organs. Gastric cancer is more common in men than in women and tends to occur mainly in older people over the age of 55.
The stomach is a hollow muscular organ, part of proximal digestive system and located on the left side of the upper abdomen below rib cage. The stomach receives food from the esophagus. It secretes acid and digestive enzymes. Gastric cancer also known as stomach cancer arises from the inner lining (mucosa) of stomach. Early gastric cancer involve only inner layer (mocosa) while in advance stage it involves more deeply into the stomach wall and spread to surrounding organs. Gastric cancer is more common in men than in women and tends to occur mainly in older people over the age of 55.

 Surgery is the most definitive treatment. Surgery is always required for curative treatment. Part or all of the stomach, as well as the surrounding lymph nodes are removed, with the basic goal of removing all cancer and a margin of normal tissue. Depending on the extent of invasion and the location of the tumor, surgery may also include removal of part of the intestine or pancreas.
Surgery is the most definitive treatment. Surgery is always required for curative treatment. Part or all of the stomach, as well as the surrounding lymph nodes are removed, with the basic goal of removing all cancer and a margin of normal tissue. Depending on the extent of invasion and the location of the tumor, surgery may also include removal of part of the intestine or pancreas.