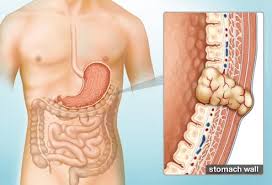
 GIST is an unknown tumor of Gastrointestinal tract (1-3% of gastrointestinal malignancies). It can develop from any part of the digestive tract from the food pipe (esophagus) to the anus and from the nearby structures to the intestine within abdominal cavity. GIST is a type of soft tissue sarcoma which arises from connective tissues of bowel wall also called interstitial cells of Cajal (ICC). The ICCs are pacemaker cells of the gut because they send signals to trigger peristalsis. GIST tumor arising from the GI tract wall can grow outside of the involved organ or inward in the lumen of intestinal.
GIST is an unknown tumor of Gastrointestinal tract (1-3% of gastrointestinal malignancies). It can develop from any part of the digestive tract from the food pipe (esophagus) to the anus and from the nearby structures to the intestine within abdominal cavity. GIST is a type of soft tissue sarcoma which arises from connective tissues of bowel wall also called interstitial cells of Cajal (ICC). The ICCs are pacemaker cells of the gut because they send signals to trigger peristalsis. GIST tumor arising from the GI tract wall can grow outside of the involved organ or inward in the lumen of intestinal.
Incidence of GIST in gastrointestinal tract –
GISTs may also develop in the membranes of the abdominal organs like peritoneum, mesentery, omentum, the liver, the pancreas, the ovaries, the uterus, and the prostate. Because these types of GISTs do not arise directly from the GI tract, they are called extra gastrointestinal stromal tumors. When a GIST grows in a location where it is not encased in the peritoneal membranes, it is said to be retroperitoneal. GISTs most commonly spread to liver, peritoneum, mesentery and omentum. GIST rarely spreads to lymph nodes 25% of Paediatric age group GIST.
Histologically, GISTs can be classified as:
Pleomorphic/mixed morphology tumors - 10%
Epithelioid cell tumor - 20%
Spindle cell tumors - 70%
Immunohistochemistry -
GISTs are typically CD117-positive in 85-95%, CD34- positive in 60-70%, DOG 1 positive in 90% and S100 -positive in10% of cases. Aggressiveness of GIST depends on the number of mitosis and tumor size (predictive of aggressive behaviour are mitotic rate greater than 5 per 10 high-power fields (HPF), size larger than 5 cm and 10 cm, and location (small bowel more aggressive than gastric GISTs). However, tumors with low mitotic index (< 5 per 50 HPF) and smaller size (2-5 cm) can also metastasize.
Risk Factors -
No known environmental, behavioural, diet or lifestyle risk factors
Age - most often seen over age of 50 years. Children are affected very rarely. Persons with inactivation of mostly in the neurofibromatosis 1 gene (NF1) inactivate and GIST
Sex - incidence of GIST is similar in men and women. Pediatric GISTs are more common in girls and young women.
Genetic mutations - The majority of GISTs show mutations in cell-surface proteins called tyrosine kinase receptors. Most GISTs show mutations in a gene that produces a growth factor receptor called KIT. A few GISTs show mutations in the gene for a closely related receptor for platelet derived growth factor receptor alpha (PDGFR a or PDGFRA). About 10-15% of gastrointestinal stromal tumors (GISTs) carry wild-type sequences in all hot spots of KIT and platelet-derived growth factor receptor alpha (PDGFRA).
Heritability -
Majority of GISTs have random genetic mutation, only a less than 5% occur as part of hereditary familial or idiopathic. These include, neurofibromatosis (NF-1), Carney's triad (gastric GIST, pulmonary chondroma and extra-adrenal paraganglioma), germline gain-of-function mutations in c-Kit / PDGFRA, and the Carney-Stratakis syndrome.
Symptoms and signs
Symptoms of a GIST vary depending on the size and location of the tumor.
Patients with smaller tumors have no symptoms.
Larger tumors may cause symptoms include -
Vague, nonspecific abdominal pain or discomfort
A painless lump in abdomen
Vomiting or diarrhea
Bowel obstruction
Bleed into the GI tract, resulting in black or tarry stools, or occasionally in vomiting of blood.
Very rarely a GIST may rupture and patient present in emergency.
Anemia and fatigue may result from chronic slow blood loss.
Weight loss
Diagnosis
Diagnosis is based on detailed evaluation of history, physical examination, endoscopy and some radiological investigations.
History and Physical examination-
The detailed clinical history and a through abdominal examination is done to check abdominal lumps.
Ultrasound scan
For large abdominal lumps ultrasound is the primary investigation, as it is easily available and check.
Endoscopy
A thin, flexible endoscope is introduced into mouth, For esophagus, stomach and small bowel or from anus ...colon. GIST arises from these structures can be easily seen. Endoscopic features of GISTs include submucosal mass displacing the overlying mucosa. Ulceration overlying mucosa and bleeding from pressure necrosis may be present.
Endoscopic ultrasound
Endoscopic ultrasound are used for the purpose of showing size and position of GIST in Exophytic GIST. This is also used to take tissue sample (FNAC or trucut biopsy). An ultrasound probe is attached at the end of the special scope which produces an image of the intestine containing the tumor and surrounding structures.
Computerized tomography (CT) scan
CT scan Provides comprehensive information regarding the size and location of the tumor, its relationship to adjacent structures and about the presence of multiple tumors and of metastatis.
Magnetic resonance imaging (MRI) scan
MRI can detect tumors and its surrounding structures
MRI Scan gives information same as in CT Scan. Additionally it gives better information of Liver metastatsis and better delineation of Pelvic GIST.
PET (positron emission tomography) scan
It is used for the assessment of metastatic disease (diseases which has spread to local or distant organs). It is also used in monitoring of response to adjuvant therapy.
 The treatment for GIST depends on many factors, like general health of the patient, the size and location of the tumor, adjacent infiltration and distant spread of the tumor. Surgical removal of the tumor is the mainstay treatment.
The treatment for GIST depends on many factors, like general health of the patient, the size and location of the tumor, adjacent infiltration and distant spread of the tumor. Surgical removal of the tumor is the mainstay treatment.
Tumors of big size that can't be removed with surgery, local involvement and those with distal spread, targeted chemotherapy to inhibit the growth of tumor is used.
Resectable GISTs can be completely removed by surgery. Therapy with imatinib mesylate is given following surgery, to decrease the recurrence, if the histopathology evidence of aggressive tumor.
Unresectable GIST cannot be completely removed by surgery because they are too large or in a place where there would be too much damage to nearby organs if the tumor is removed. Treatment is usually targeted therapy with imatinib mesylate to shrink the tumor, followed by surgery to remove as much of the tumor as possible.
Metastatic GIST may include the targeted therapy with imatinib mesylate or sunitinib, or sonafiaib if the tumor shows signs of resistance to imatinib mesylate therapy or if the side effectsare too bad. Surgery is planned if tumor shrinks.
 Surgery is performed by either open or minimally invasive methods. Minimal invasive methods has less post operative morbidities, less pain, short hospital stay and less wound complication. Preference of the methods of surgery depends on the size of tumor and the availability of the expert. Surgery is the best treatment for GIST. In localized, resectable adult GISTs, if anatomically and physiologically feasible, surgery is the primary treatment of choice. Lymph node metastases are rare, and routine removal of lymph nodes is typically not necessary.
Surgery is performed by either open or minimally invasive methods. Minimal invasive methods has less post operative morbidities, less pain, short hospital stay and less wound complication. Preference of the methods of surgery depends on the size of tumor and the availability of the expert. Surgery is the best treatment for GIST. In localized, resectable adult GISTs, if anatomically and physiologically feasible, surgery is the primary treatment of choice. Lymph node metastases are rare, and routine removal of lymph nodes is typically not necessary.
The tumor is resected along with some surrounding healthy tissue. If the tumor has begun to grow into other tissues close by, these are also removed.
Sometimes isolated secondary tumors are removal if feasible.
For gastric GIST, depending upon the size, location a part or most of the stomach is removed.
For small bowel GIST, the loop containing the GIST is resected and the continuity of bowel is restored.
Surgery is done to remove tumors when there are serious complications, such as bleeding, a hole in the gastrointestinal tract, a blocked GI tract;
Targeted Chemotherapy (Growth inhibitors)
In about 85% of people with a GIST, the tumor cells have a change (mutation) in KIT. Treatment with growth inhibitors can block these signals. This may make the cancer shrink or stop it from growing. Growth inhibitors may be used to treat GISTs that can't be completely removed with an operation. These are imatinib and sunitinib.
The side effects of imatinib include tiredness, feeling sick (nausea), diarrhoea, swollen ankles and puffy eyes, and an itchy rash. Common side effects of sunitinib include a skin rash and soreness, tiredness, mouth ulcers and high blood pressure. These side effects can usually be well controlled with medicines.
Follow-up
Follow-up for GISTs that were removed by surgery may include CT scan of whole abdomen to see the local recurrence as well as distal metastasis. For GISTs that are treated with tyrosine kinase inhibitors, follow-up tests, such as CT, MRI, or PET scans, may be done to check how well the targeted therapy is working.